Basal cell carcinoma is a type of skin cancer that begins in the basal cells, which produce new skin cells when the old ones die off. Basal cell carcinoma is the most common type of skin cancer. About 3.5 million cases of skin cancer are diagnosed each year, with eight out of ten of those cases being basal cell cancers.
Symptoms
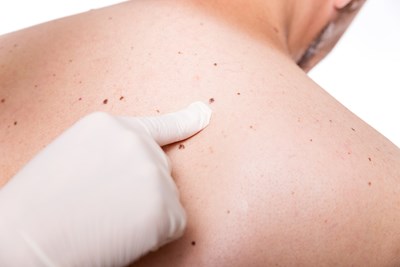
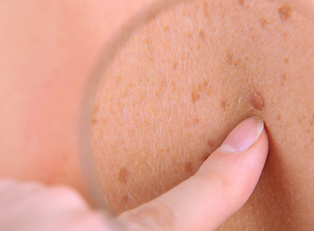
Basal cell carcinomas will generally develop on parts of your body that are often exposed to the sun, such as your head and neck. However it is possible for the cancer to appear on parts of your body that are rarely exposed to sunlight, such as your trunk and legs. Some general warning signs of basal cell carcinoma include:
- A sore that won’t heal
- A flat, scaly, brown or flesh-colored patch
- A pearly white or waxy bump (For people with darker skin, these bumps may appear brown or black)
- A white, waxy scar
Causes and Risk Factors
Basal cell carcinoma is caused by a mutation that has developed in the DNA of basal cells. The mutation causes them to multiply rapidly and continue growing when they should die. This accumulation of abnormal cells will eventually result in a cancerous tumor.
The main cause of these mutations is an overexposure to ultraviolet radiation found in sunlight, tanning lamps, and tanning beds. However, this doesn’t account for skin cancers that develop in areas that are not exposed to UV light. Other factors that can increase your risk for basal cell carcinoma include:
- Chronic sun exposure: The risk is higher if most of your exposure is before the age of 18.
- Radiation exposure: If you have undergone radiation treatments for any reason, such as psoriasis or childhood acne, this will increase your risk.
- Fair skin: People with fair skin that freckles or sunburns easily are more likely to develop skin cancer than people with darker complexions.
- Sex: Men are more likely to develop basal cell carcinoma than women.
- Age: The majority of basal cell carcinoma cases occur in people age 50 or older.
- Family history: If someone in your immediate family has had basal cell carcinoma in the past, this will increase your risk as well.
- Personal history: If you have had basal cell carcinoma before, your risk for developing it again in the future will be greater.
- Immunosuppressive drugs: If you are taking medications to suppress your immune system, such as those taken after transplant surgery, your risk will be increased.
- Arsenic exposure: Arsenic is a toxic metal that increases your risk of certain cancers, including basal cell carcinoma.
Treatments
Once you have been diagnosed with basal cell carcinoma, you and your doctor will decide on the treatment plan that works best for you. Common treatment options include:
- ED&C: This is a procedure called electrodesiccation and curettage, and it involves removing the surface of the skin cancer with a scraping instrument and searing the base of the cancer with an electric needle.
- Surgical excision: This involves cutting out the cancerous tissue, as well as a surrounding margin of healthy skin to prevent spreading.
- Freezing: This involves killing the cancerous cells by freezing them with liquid nitrogen.
- Topical treatments: Some creams and ointments can be used to treat basal cell carcinomas that do not extend very far into the skin.
- Medications: If the cancer has spread to other parts of the body, it may be treated with other medications.