Ankylosing spondylitis is a painful condition that causes the vertebrae of the spine to fuse together. Since its symptoms are similar to those of more common back problems and develop rather gradually, many people delay being examined by a doctor. Additionally, there is no official diagnostic test for this disease. This combination of delay and lack of necessary tests means that some patients may live with symptoms for a decade or more before their doctors realize that they’re suffering from AS.
Thankfully, physicians are still able to piece together a diagnosis (albeit slowly) by running a series of examinations that may help point them in the right direction. Here is a look at some of those tests.
Physical Assessment
One of the first things doctors will normally do is ask the patient about their physical symptoms. Ankylosing spondylitis tends to cause sufferers more back pain at night and in the early morning, so they’ll be particularly interested at the specific time of day when the symptoms occur. They will also probably ask questions about physical activity levels, since exercise can often provide relief from back pain caused by AS.
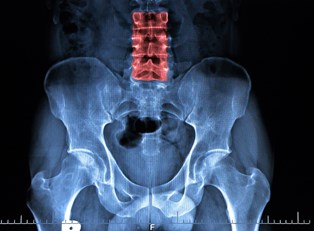
X-Rays
Over time ankylosing spondylitis erodes the patient’s sacroiliac joint (the joint that connects the spine to the hips), so doctors will recommend X-rays to examine whether or not this damage is taking place. Unfortunately, damage only becomes severe enough to detect after seven to 10 years of suffering from AS, so it may not show up if X-rays are taken sooner than this.
Genetic Testing
A majority of people suffering from ankylosing spondylitis have a specific gene in common: HLA-B27. While researchers are still unsure about the role it plays in the AS process, they’re confident that it does serve some function since so many people with the condition carry it. However, it should be noted that the presence of this gene is not a surefire indicator that someone will develop the disease.