There is no cure for diabetic neuropathy, and by the time you experience symptoms, extensive nerve injury may have already occurred. As a result, treatment is focused on managing your symptoms and addressing any complications caused by your neuropathy.
It isn’t yet clear whether diabetic neuropathy is completely preventable, but experts say that regulating glucose levels and maintaining a healthy diet, weight, and lifestyle can slow down the process of nerve injury. These practices may also slow down or prevent neuropathy from spreading or worsening once symptoms are manifested as well.
Diabetic neuropathy can affect any nerve in the body. Symptoms and treatments will vary according to where the nerve damage takes place. Here are some common approaches to treatment:
- medication
- assistive devices
- behavior modification programs
Medication
Insulin injections and oral pills may be used for managing hyperglycemia (too much glucose in the blood). Drugs that help control blood pressure, cholesterol levels, and other heart medications can help improve circulatory issues that lead to diabetic neuropathy. Analgesics, opioids, and antidepressants are often given for pain management. Antidepressants can also help diabetics cope with depression and social isolation. Medications are also given to treat digestive issues and sexual disfunction caused by diabetic neuropathy.
Assistive devices
As neuropathy affects the eyes, glasses or contacts may be needed for adjustment to changes in vision. When erectile disfunction results from nerve damage to the sexual organs, patients may receive help from penile vacuum devices that increase blood flow to the penis and assist with producing erections.
Devices such as canes, walkers, foot and leg braces, or wheelchairs may be required by patients suffering from neuropathy that affects the toes, feet, and legs. As these patients experience the loss of feeling, the ability to move the toes and feet, or leg strength, they may frequently trip and fall when walking without assistance.
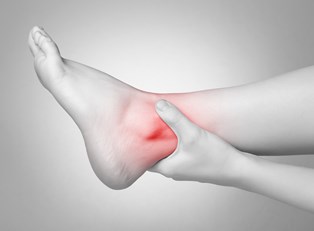
A number of patients experience sharp pain in their toes and feet. Even the light weight of a bed sheet can result in unbearable pain. These patients may require a mechanical device called a bed cradle that allows the bed clothes to hover over the feet without touching them.
Behavior modification programs
Diabetics who smoke or consume alcohol may be enrolled in smoking cessation programs or be encouraged to join alcohol abuse support groups that provide support and information for stopping these dangerous habits that can contribute to neuropathy.
Many diabetics, especially those with type 2 diabetes, may attend classes that encourage ways to reduce the fat, fiber, or the amount of calories in their diets. Programs such as these will encourage heart-healthy weight management practices. Other patients receive therapies that help them learn new swallowing techniques.
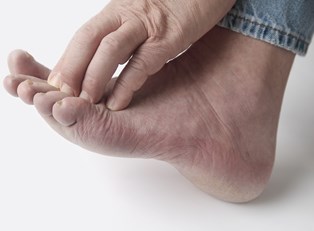
Peripheral neuropathy, or nerve damage in the extremities, is the most common form of diabetic neuropathy. The toes and feet are most commonly affected. Foot care is critically important for all diabetics, but especially for those with peripheral neuropathy. Due to a limited circulation to the feet and a loss of feeling, many patients with neuropathy can develop and not notice wounds on the feet that may become seriously infected. When left untreated, these may become life-threatening and require amputation.
It is a good idea to look over your feet and between your toes everyday. You’ll want to look for swelling, blisters, cracks in the skin, sores, and changes in color. Hand follow these tips:
- wash your feet with mild soap and lukewarm water everyday, drying them thoroughly
- moisturize your skin with lotion to prevent cracks in the skin
- avoid burns by always checking the temperature of bathwater or standing water before stepping into the shower or bathtub
- never walk around barefoot
- shake your shoes out before putting them on
- wear shoes that match the shape of your feet and that do not constrict them
- put on a fresh pair of padded, loose-fitting, and breathable socks everyday
- do not open blisters
- carry a first aid kit with you when you travel
- trim toenails after bathing, when they are soft
- trim toenails straight across and file them with an emory board
- never trim your cuticles
Asking your doctor for information on preventing injuries and maintaining good foot health is strongly recommended. Your physician may want to check your feet at every visit and inspect them thoroughly once a year. Any changes related to your feet should be discussed with your health care provider.