CT Scan
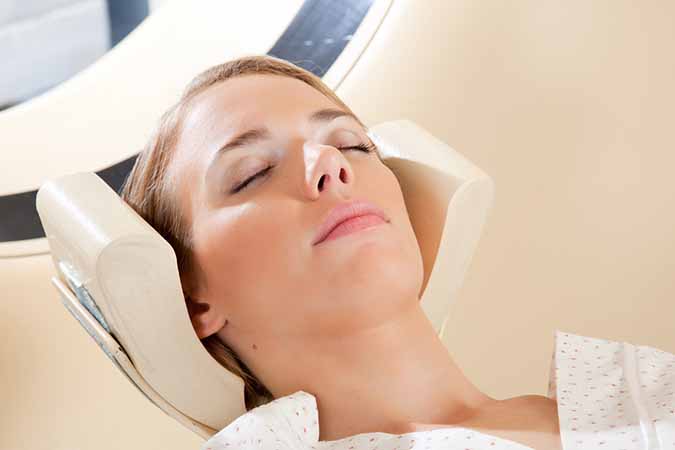
When doctors recommend a full body CT scan, it’s important to ask questions to find out if it’s really necessary. CT scans are one of the largest contributors to radiation exposure and can result in a greatly increased risk of death by cancer. In most cases, a traditional X-ray can be less dangerous and more informative.
The CT scan, or computerized tomography scan, uses a series of X-ray images taken from different angles around your body, which are then processed through a computer to create a full image that is much more detailed than a typical x-ray. As such, you are exposed to more radiation than you are with a regular x-ray image.
Organ Transplant
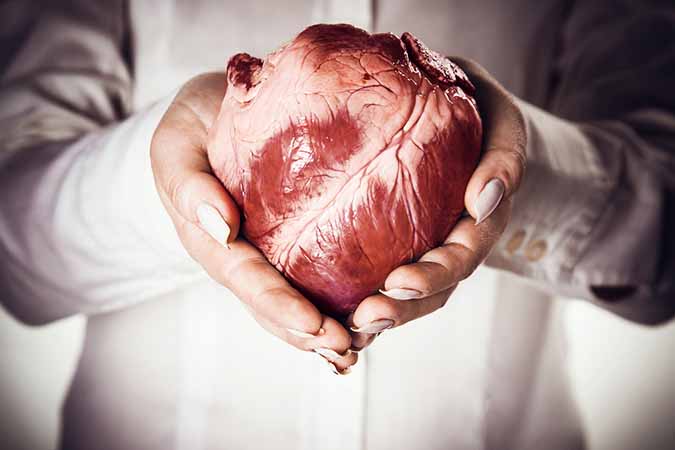
Patients requiring any sort of organ transplant are already in poor health, which immediately increases the inherent surgical risks. Once the transplant is complete, the most serious complication is the fact that the body may reject the new organ. According to the John Hopkins School of Medicine, liver and intestinal transplants present the highest risk of all.
After organ transplant surgery, a number of different complications can ensue. In addition to the body potentially rejecting the organ, immunosuppressant drugs given to the patient can increase their risk of infection or disease. Potentially, a patent may be exposed to diseases such as hepatitis B, HIV or even cancer from the donor organ itself.
Epilepsy Surgery
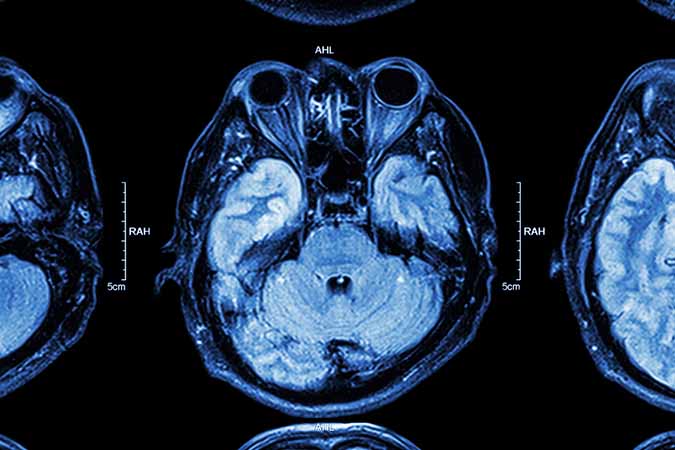
While some people with epilepsy face seizures only occasionally, others may have up to a hundred over the course of 24 hours. Medication is typically the first course of action, but when that fails, surgery may be suggested. It's usually a last resort, however, due to the risks involved with it.
It may be highly effective for some, but it also has the potential to leave patients with serious motor impairments, paralysis, memory loss, or even increased seizures. Brain surgeries of all types most certainly come with the highest risks of any surgical procedure. However, there is a great deal of testing done before the surgery to ensure that it will help more than harm the patient.
Breast Reduction

Physically, there’s always the potential for scarring or poor workmanship when getting a breast reduction. One of the most common is decreased sensitivity in the nipple area, which occurs up to 70% of the time. Additionally, there's a chance that you could experience tissue necrosis (aka tissue death), excessive firmness, deep vein thrombosis, or persistent pain.
There's also a risk of allergic reaction to the tape, sutures, topical preparations and injectable agents used during the surgery. After the surgery, breast reduction also has a chance to interfere with certain diagnostic procedures, limit the ability to breastfeed, and can alter the outcome after pregnancy. Breast asymmetry and excessive firmness may develop as a result of the surgery.
Transvaginal Mesh

Resulting in thousands of lawsuits, transvaginal mesh was originally intended to help women with vaginal prolapse and stress urinary incontinence. However, the FDA finally declared it was doing more harm than good. Studies show that side effects such as tissue erosion and organ perforation occur at an alarming rate and generally negate the potential benefits of transvaginal mesh.
Transvaginal mesh surgery involves making an incision on the vaginal wall. Mesh is then inserted at the point of incision to assist in holding up the fallen organs. The aim was for tissue to grow into the holes of the mesh, creating a supportive barrier. In addition to the United States, the surgery has been banned in numerous other countries.
Gastric Bypass

The main risk of gastric bypass is the weight of the patients. Most medical procedures are riskier on someone who is overweight, and larger patients are also more susceptible to postsurgical problems, such as pneumonia. Excessive bleeding, infection, gastrointestinal leaks and blood clots are just some of the risks involved.
During gastric bypass, it can be difficult to find a vein to administer IV fluids, more anesthetics may be necessary, and there are layers of fat that have to be gone through in order to reach the stomach. Some patients will have adverse reactions to the anesthesia and breathing difficulties may also develop during the procedure.
Spinal Tap

Spinal taps are used to detect meningitis, bacteria, bleeding, and other debilitating diseases related to the spine and brain. The patient is poked with a lumbar puncture straight into the spine, and cerebrospinal fluid is then removed and tested. During a spinal tap, dyes or radioactive substances may be injected into the spine in order to take diagnostic images of the spine.
Spinal taps can cause nerve paralysis even when done right, and when done wrong, total paralysis may ensue. Around a quarter of patients who receive a spinal tap will suffer from a post-lumbar puncture headache due to spinal fluid leakage into nearby tissues. This headache can last anywhere from several hours and up to two days.
Cesarean Section
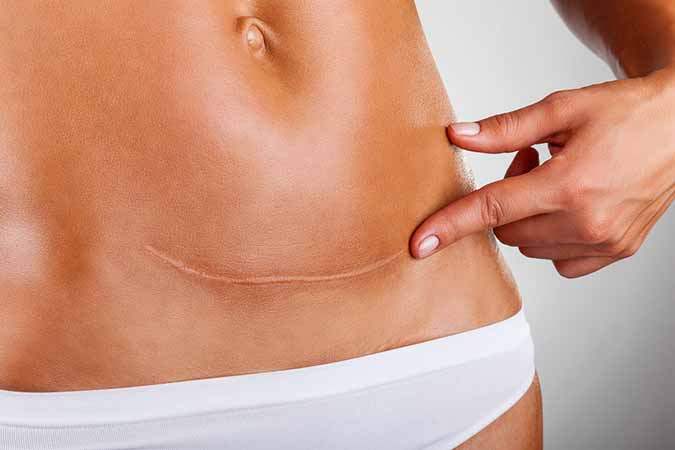
Sometimes a C-section is absolutely necessary for the safety of a mother and her baby. However, if it isn’t a medical necessity, it may not be worth the risk. First and foremost, once a woman has a c-section, she’s going to need one for every subsequent birth and that means the same risks each and every time.
As with any surgery, risk of infection may occur. Excessive bleeding and blood clots are other potential risks. Additionally, one wrong move with a scalpel can hit nerves, leaving a mother in excruciating abdominal and vaginal pain for months—not necessarily the easiest thing to deal with while trying to take care of a newborn.
Circumcision

“High risk” may be a little bit of an exaggeration, but the fact of the matter is, outside of religious reasons, circumcision is largely unnecessary. Furthermore, circumcised boys have less penis sensitivity than males who don’t have the procedure. And when the surgery goes wrong, which is admittedly rare, serious problems may arise—such as infection, bleeding, or genital loss.
The benefits of circumcision are said to be easier hygiene and decreased risk of urinary tract infection and STIs. But these things can all be prevented with careful hygiene. The risks of the procedure going wrong may not be preventable such as improper healing or the foreskin being cut too short or too long.
Cancer Operations

Some candidates that have cancer are able to have their cancer removed via surgery. While it may seem easier than chemotherapy, it comes with risks. The surgery can involve removing an entire organ or group of tissues while even the simplest cancer operation requires meticulous searching for every bit of cancer inside the body.
Dangers lie in infection, loss of organ function, bleeding, blood clots, and the risk that all the cancerous cells may not have been completely removed. During cancer surgery, there is also a risk of damage to nearby tissues and a reaction to drugs administered during the procedure. Recovery times will vary as well.
Brain Surgery
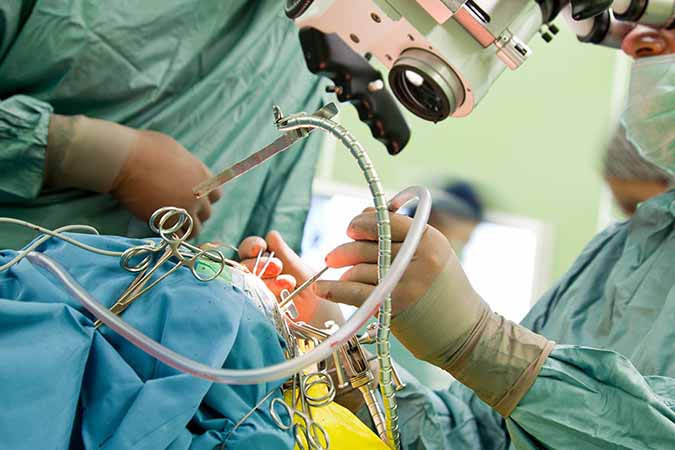
Without a doubt, the most dangerous type of medical procedure in the world is brain surgery. These surgeries require removing part of the skull to reach the brain, and sometimes the piece isn’t replaced for several days, like in the case of swelling of the brain. Infection is the biggest risk, which can be deadly given it already starts in the brain.
Brain surgery can lead to brain damage which can cause permanent impairment or brain death. A speech-language pathologist may test you before and after surgery in order to compare results and determine whether any brain damage or improvements have occurred. Images will also be taken before and after surgery as well.
Abdominal Exploration
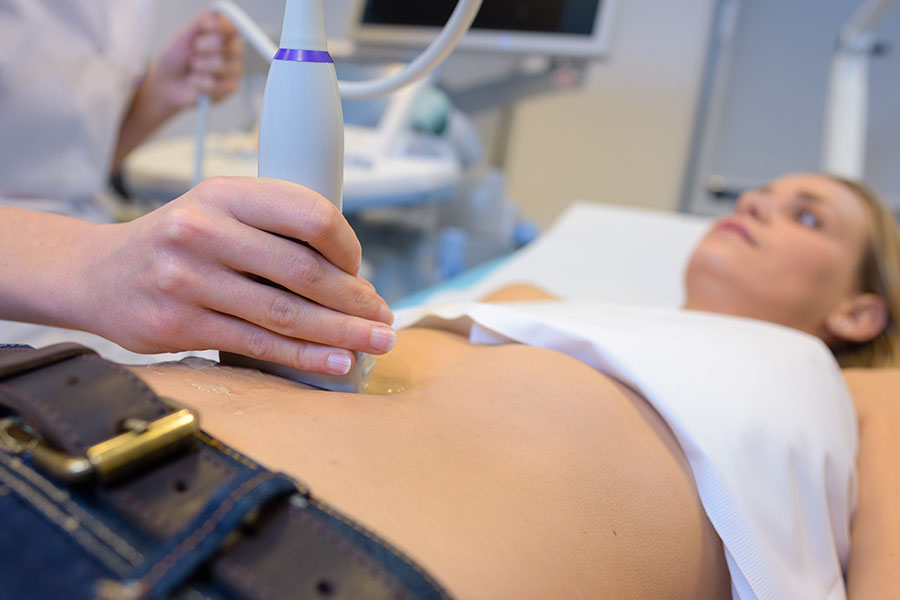
Abdominal exploration is more common than you’d think. Many are listed as other reasons when the issue is discovered and repaired, but this type of medical procedure has a high mortality and complication rate. For this reason, it’s important to ask if an abdominal exploration is absolutely necessary when a doctor suggests it.
Abdominal exploration is a surgical procedure for looking at your organs and other structures in your belly area such as your liver, pancreas, kidneys, gallbladder or intestines. The surgery for opening the abdomen is called a laparotomy and during that procedure, you are usually under general anesthesia which comes with its own risks.
Pancreatectomy
A pancreatectomy is when the pancreas is partially or completely removed. According to a John Hopkins study, a terrifying 41% of these surgeries ended with complications. One of the most serious is bleeding post-op, which made food and liquids slow to leave the stomach but this is just one of the complications that can occur.
A fistula, which is a leak, can occur when the sutures fail to seal correctly. When this occurs, you may need to be fed intravenously until the tissue has healed. Losing part of your pancreas can also mean an increased risk of diabetes since the purpose of the pancreas is to release insulin.
Penile Enlargement

When pumps, creams, and pills don’t work, some men turn to surgical options to enhance their manhood. While there are a few different methods to increase length or girth, there haven’t been nearly enough studies done to prove efficacy, and no prominent medical organization endorses them, particularly if the penis is already an adequate size.
In severe cases, these surgeries can result in less sensitivity, erectile dysfunction, and nerve damage. Additionally, it’s also possible that the scarring from the surgery may actually make the penis shorter. Ultimately, the risks of deformity and dysfunction may make the surgery not worth the risk when the surgery is not necessary.
Stents

In most cases, a stent isn’t an option for someone that needs it. They’re installed to open up a clogged artery, but some professionals suggest they’ve been overused in recent years in cases where medication may have been enough. Stents are permanent and if the narrowing of the artery continues, another stent can be placed.
Some of the most common risks of stents occur from the surgery itself, but you can also have an infection of the vessel. Other risks include a blockage in the artery, re-narrowing of the vessel, and blood clots. These complications can potentially lead to life-threatening events like a heart attack or stroke.
Septal Myectomy
A septal myectomy is a type of open-heart surgery to reduce the thickening of the muscle. The goal being to reduce the symptoms of hypertrophic cardiomyopathy. Most surgeries involving the heart are terrifying, but this one is particularly scary. The risks of this procedure are potentially life-threatening, which include infection, heart attack, stroke, and death.
However, patients that undergo this surgery have a much higher chance of survival (compared to those choosing to opt out), making it a necessary but frightening surgery. The surgery has been performed for many years and it is relatively safe for that reason but risks vary depending on the person.
Thoracic Aortic Dissection Repair
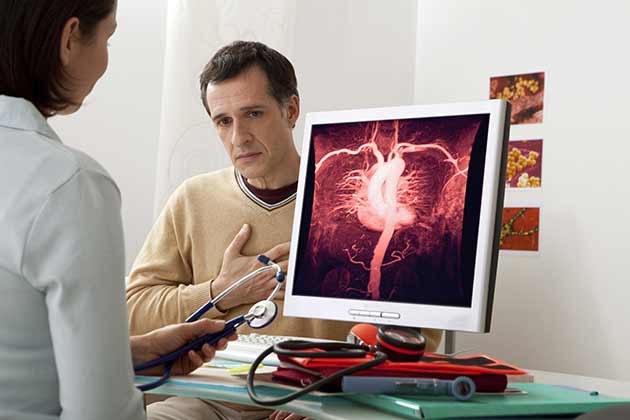
An aortic dissection is a tear in the wall of the body’s main artery, the aorta. This particular procedure repairs the portion of the aorta that runs through the chest. The surgery itself can trigger a number of complications, including heart failure, stroke, and a further rupture in the aorta.
A thoracic aortic dissection repair is not truly an optional surgery. It's a medical emergency that requires immediate treatment. You'll be under general anesthesia during the procedure and your vital signs will be under watch during the duration of the procedure. After the surgery, it can take months to fully recover.
Esophagectomy
Esophagectomy is a procedure to remove part or all of the tube that connects your mouth to your stomach while also reconstructing it using some of another organ. The risks can range from mild to severe and can include infection, cough, hoarseness, acid or bile reflux, respiratory influx, and difficulties swallowing.
An esophagectomy is most commonly used to treat esophageal cancer but can also be used to treat conditions like Barrett's esophagus. In many case, an esophagectomy can be done as a minimally invasive surgery, however, in other cases, an open esophagectomy may be necessary, in which case a surgeon removes all or part of the esophagus and replaces it.
Bladder Cystectomy

A bladder cystectomy is necessary to remove part of (or all) of the bladder. A common risk with these types of surgery includes infection and bleeding, but an infection could lead to peritonitis. Patients can also experience leakage from the bladder incision site, which can cause several other internal problems.
A bladder cystectomy that involves the removal of the entire bladder is called a radical cystectomy. When this occurs, the surgeon will have to design a new way for you to store urine and provide a way for it to leave the body, which is called urinary diversion. The reason for this procedure is most commonly bladder cancer that is recurring or has invaded the muscle tissue.
Removal of Abdominal Adhesions

After intestinal surgery, patients can develop painful scar tissue months or years later, and it must be removed via surgery. Complications can include a tear in the bowel, and there’s a chance it won’t alleviate the pain. Many doctors are choosing not to complete this surgery on their patients.
Removal of abdominal adhesions will require a great deal of recovery time. You may feel weak and tired after surgery and potentially suffer from nausea or stomach ache. Pain in the abdomen may last up to weeks. This is the best case scenario. The risks of the procedure include damage to the organs, infection, bleeding and even hernia.
Stomach Ulcer Surgery

Anyone with peptic ulcers can tell you that they’re incredibly painful. These are open sores that develop on the lining of the stomach. Often, these sores will heal on their own after a few months but they may need to be treated with antibiotics or a proton pump inhibitor depending on the cause.
Ulcers caused by NSAIDs are usually treated with a proton pump inhibitor, while ulcers caused by bacterial infection are treated with antibiotics. Sometimes, these ulcers need to be controlled with surgery. This type of surgery isn’t very common because it has exceptionally high risks of complications and mortality. Nausea, pain, vomiting and fever may occur after surgery.
Back Surgery

Nearly all back surgeries carry a large risk. While helpful, it can have a number of complications that will affect a patient’s quality of life. Some of the risks include infection, blood clots, heart attack, stroke, and nerve damage. The nerve damage can result in weakness, paralysis, pain, or loss of bowel or bladder control.
Back surgery may be required for a number of reasons. Herniated or ruptured disks, spinal stenosis, fractures and degenerative disk disease are just some of the reasons a doctor may want to perform surgery. Because the spine is connected to the central nervous system, it's one of the riskiest categories of surgery.
Colectomy
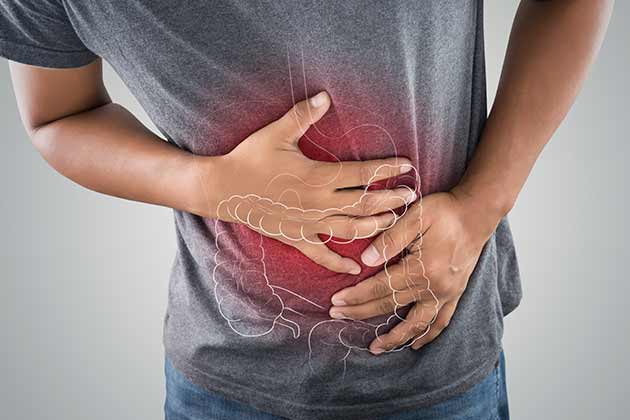
A colectomy is used to remove parts or all of the colon. As with any bowel surgery, risks scar tissue and injury to surrounding organs. Another terrifying risk is leaking at the incision site, which can cause a leakage inside your body. This can cause infections that can be extremely deadly.
A colectomy may be performed for a variety of reasons. Uncontrollable bleeding of the colon may require a partial removal of the colon while bowel obstruction may require a partial or total removal of the colon. Colon cancer, ulcerative colitis, Crohn's disease and recurring diverticulitis are, among other reasons, why a colectomy may be needed.
Laparotomy
A laparotomy is a surgical incision into the abdominal cavity that uses a full-sized incision rather than a minimally invasive approach. This type of procedure is done for a few reasons, from abdominal exploration to a patient that’s had a stroke. A laparotomy carries a high mortality and complication rate.
A number of things can go wrong during surgery. There may be damage to the internal organs. Pain, infection, bleeding, and bowel blockages may also occur. After your surgery, you'll basically be out of commission for a while. You will likely not be able to eat for a few days, you will need to walk around to prevent blood clots and your vitals will be monitored. After you are discharged, you'll be instructed to rest as much as possible in the first couple weeks, you will have to follow a modified diet, continue exercise and take medications as directed.
Conjoined Twin Separation

This isn’t a surgery many people undergo—it’s actually extremely rare. However, that doesn’t mean it isn’t risky. Most often, conjoined twins share one or more organs, which risks the death of one or both patients. There are instances of successful surgeries, but it isn’t uncommon for patients to pass during separation.
Conjoined twin births occur every 50,000 to 60,000 births. Among conjoined twins, around 75% of them will share organs with one another. Only if twins have their own separate organs are the chances of survival higher. Twins that share a heart cannot be separated. According to CNN Health, only 75% of separation surgeries result in at least one surviving twin.
Craniectomy
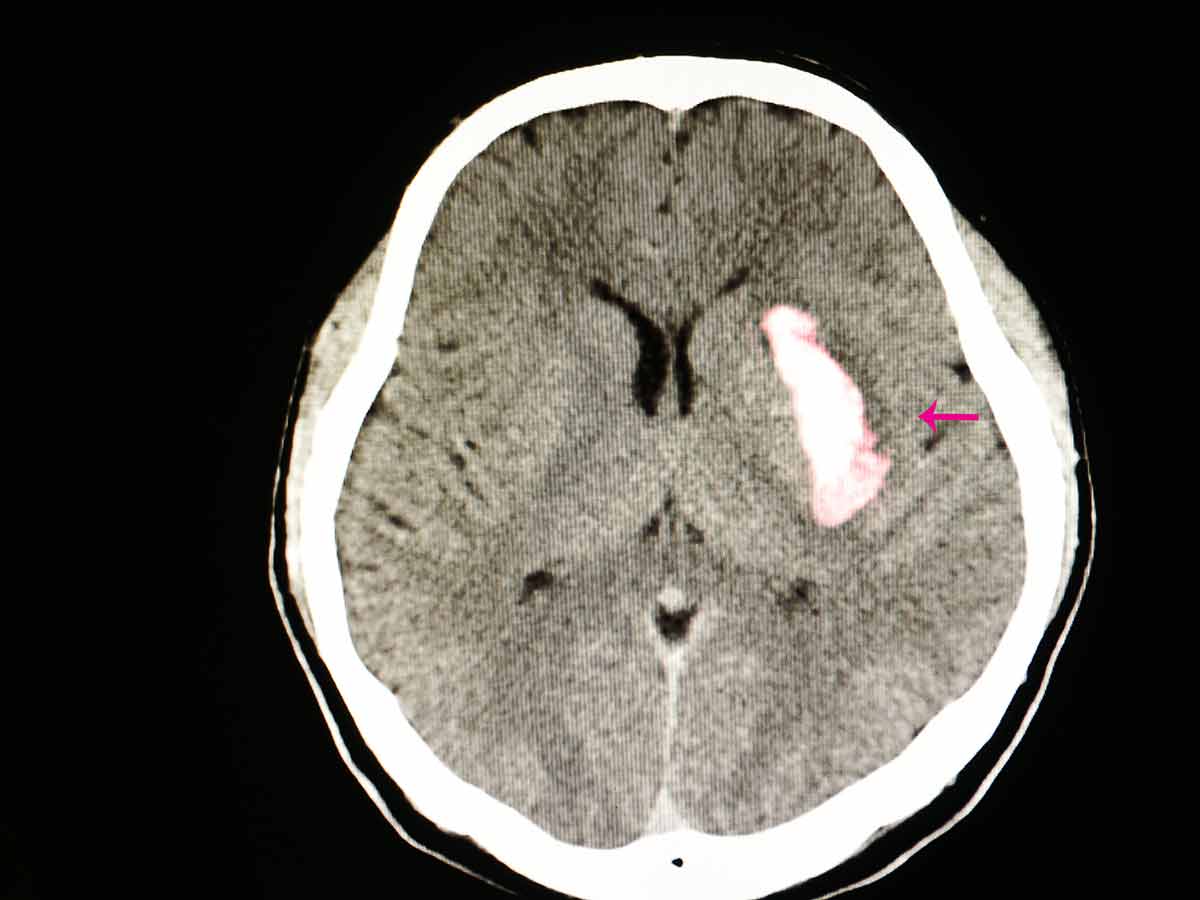
A craniectomy is an intense but sometimes life-saving procedure where a portion of a patient's skull is removed entirely. This is typically done when someone has experienced a severe head injury that has caused swelling and bleeding on the brain. Holes are first drilled into the skull, and then those are connected by cuts with a saw, and finally, a portion of the skull is removed.
It doesn't take a medical doctor to realize that removing a portion of your skull is a highly risky procedure. Complications of a craniectomy can include bleeding and infection in the brain. While these risks are high, most patients undergoing a craniectomy have already suffered severe brain damage and could die without treatment, which often skews the risk assessment in favor of this procedure.
Surgical Ventricular Restoration
Patients who have experienced extreme heart failure may be offered surgical ventricular restoration as a means of treating damage done to the organ. The procedure involves making incisions into and inflating the heart to correct any deformations in it created by scar tissue. While this can be lifesaving, it's not without risks.
At the time of the procedure, survival rates of surgical ventricular restoration are very high. However, if surgical ventricular restoration is done in conjunction with other procedures (like bypass surgery), this will increase the amount of stress on the heart and the potential for complications. The real risks come in the long term—patients who undergo surgical ventricular restoration are at a higher risk of a heart attack in the future.
Coronary Artery Bypass Graft
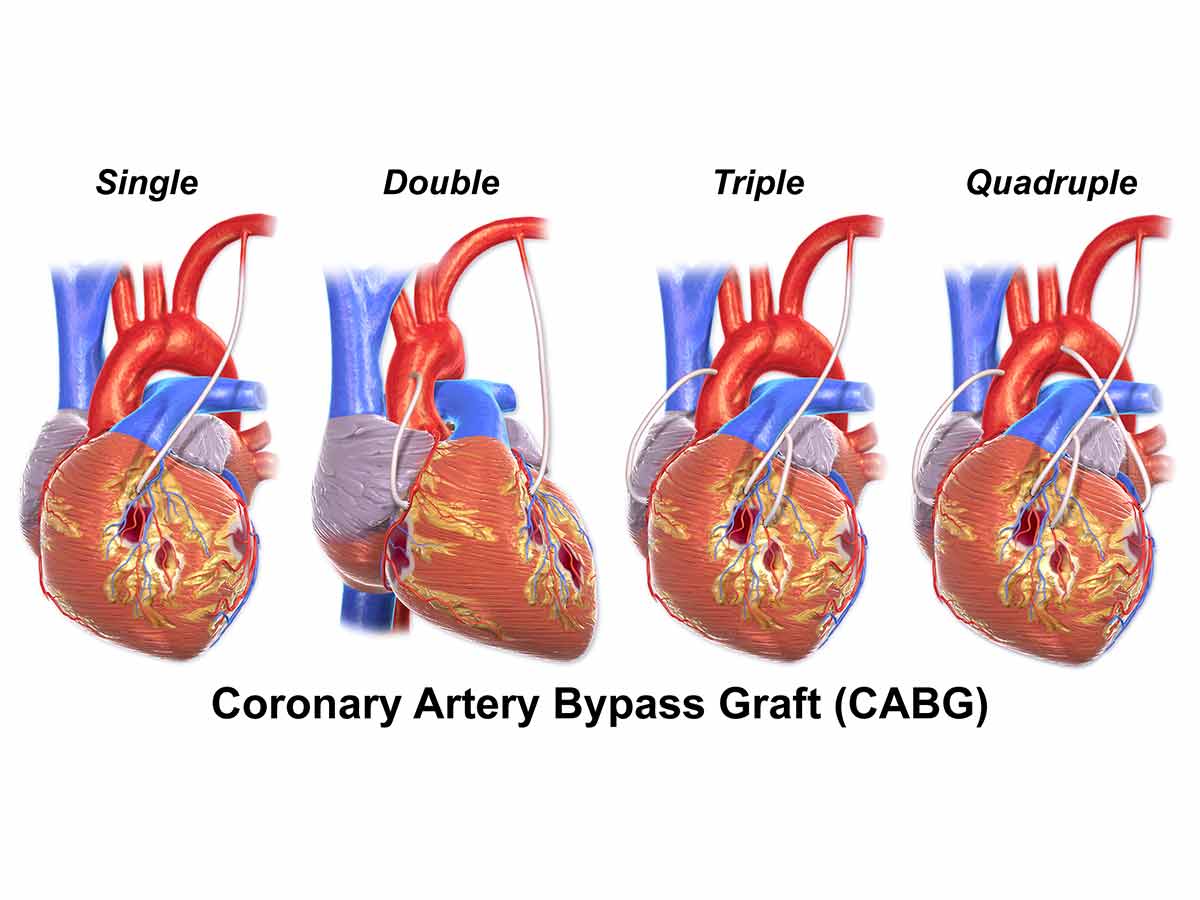
Coronary artery bypass grafts (also known as coronary revascularization) are one of the most common medical procedures in the United States, but it's also one with some of the highest risks. During the procedure, doctors identify areas in arteries narrowed by plaques. Then, healthy blood vessels are removed from other parts of the body and grafted onto the affected coronary arteries.
The surgery is complicated because of the blood vessel removal and grafting process, but most complications involve the heart and not the area of the body where healthy blood vessels are removed. These complications include an increased risk of blood clots, stroke, and heart attack. There is also the risk that the patient's body will reject the grafted blood vessels.
Epidural Steroid Injections
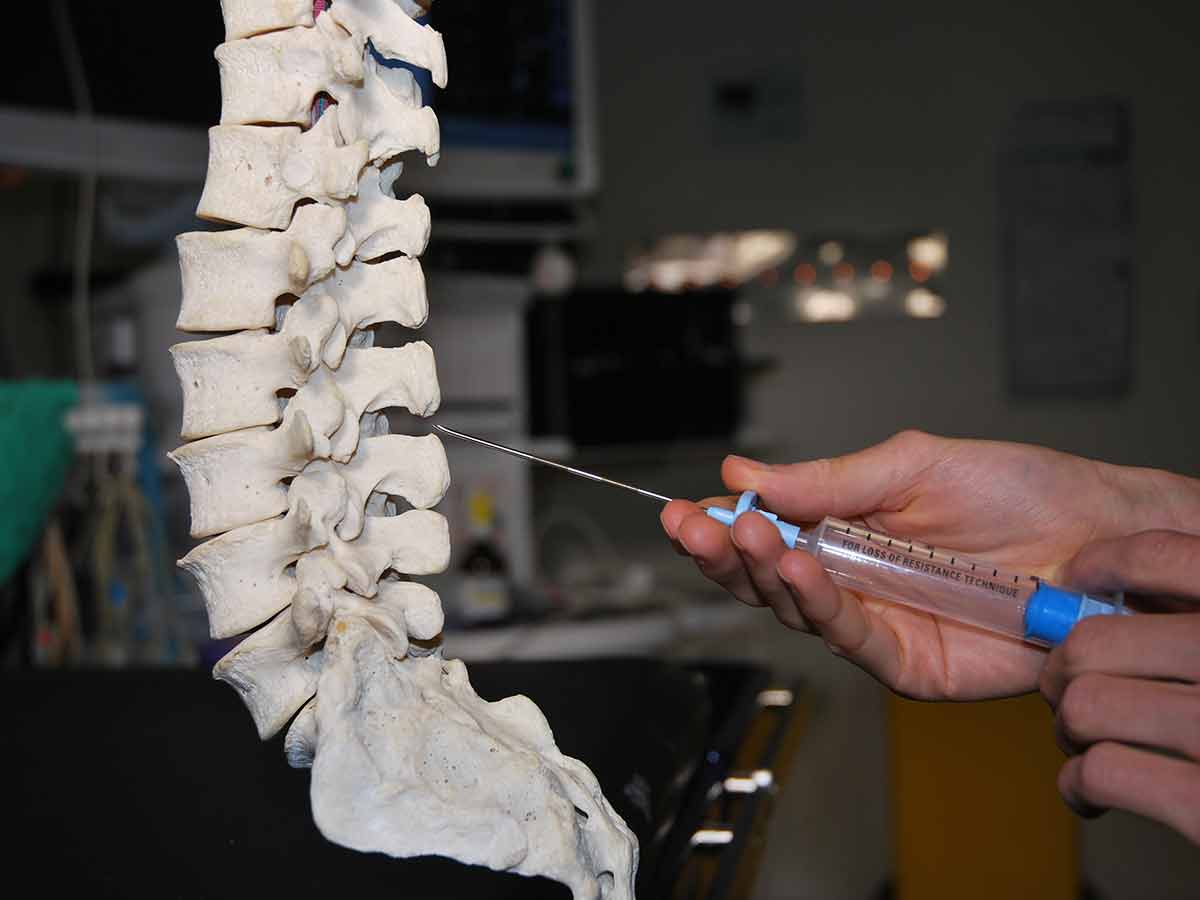
Some people experience back and neck pain that's so intense they'll do anything to relieve it. However, some of these treatments are not without risk. While epidural steroid injections can help relieve back and neck pain in the short term, it's not useful as a long-term solution and poses some serious risks.
These epidural injections are performed by making injections directly into the spinal column. This can lead to issues like paralysis, stroke, and even meningitis. Steroid injections are not riskier than any other form of epidural injection, but it's considered to be riskier since this treatment has been proven to be ineffective at treating chronic back pain. It's all risk and no reward.
Amniocentesis
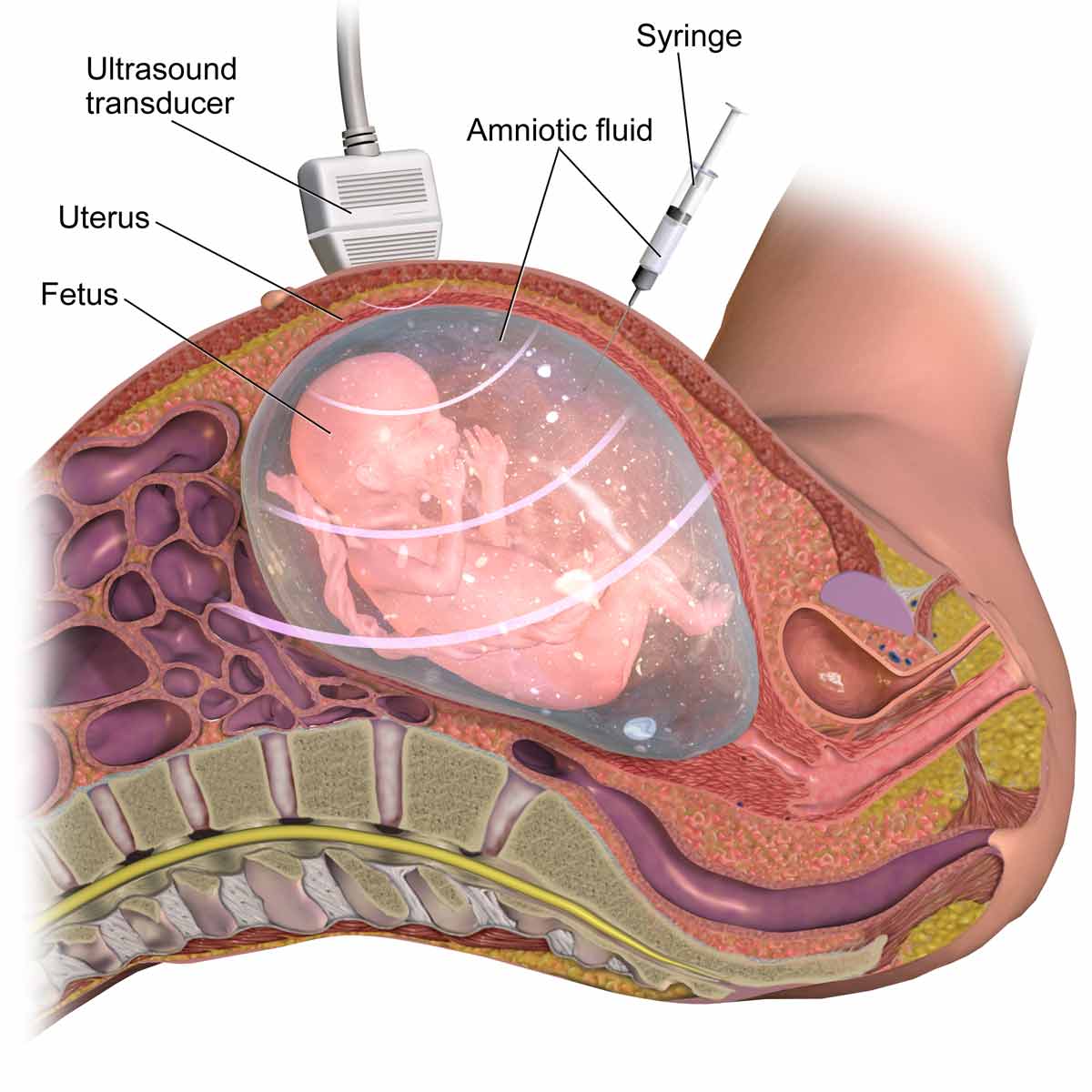
Amniocentesis is a medical procedure sometimes used on pregnant women to test for genetic abnormalities in their babies. The procedure involves removing a small amount of fluid from the amniotic sac and testing it for signs of genetic defects. While this procedure can very accurately diagnose genetic issues, it's still a risky procedure.
The rate of miscarriage among women who undergo amniocentesis ranges from 1 in 300 to 1 in 500. Because of this, the procedure should only be a last-ditch effort for instances where doctors are very concerned about severe genetic defects. In other cases, there are safer methods for uncovering any issues with the child.
Thyroid Removal Surgery
The risks of thyroid removal due to the detection of cancer are not an extremely high-risk procedure. While it does carry some risks (like all surgeries), your odds of pulling through are still very good. The real problem with this procedure is that it's often not needed, exposing patients to a low (but completely unnecessary) risk of complications.
Many medical experts have begun to express doubts about the necessity of some cancer-fighting procedures, especially when it comes to thyroid removal. They argue that many forms of cancer are so slow-growing that removing the affected organ is riskier than waiting to see if the cancer spreads and worsens. Some studies from Japan have indicated that a large percentage of patients with small thyroid tumors don't experience any growth in them.
Arthroscopic Knee Surgery
Arthroscopic knee surgery involves inserting a small camera into the patient's body via an incision near the knee and using that footage to repair a torn meniscus. While the surgery is minimally invasive and low risk, this is another instance where the riskiness of the procedure comes from the fact that it's frequently ineffective and unnecessary.
Arthroscopic knee surgery has become a more common treatment for people dealing with arthritis in their knees. However, studies have shown that this procedure is only effective at treating pain from acute meniscus injuries—it's been shown to be much less effective at treating pain that comes from age and use (as is the case with arthritis).
Prostate Cancer Screenings & Surgery
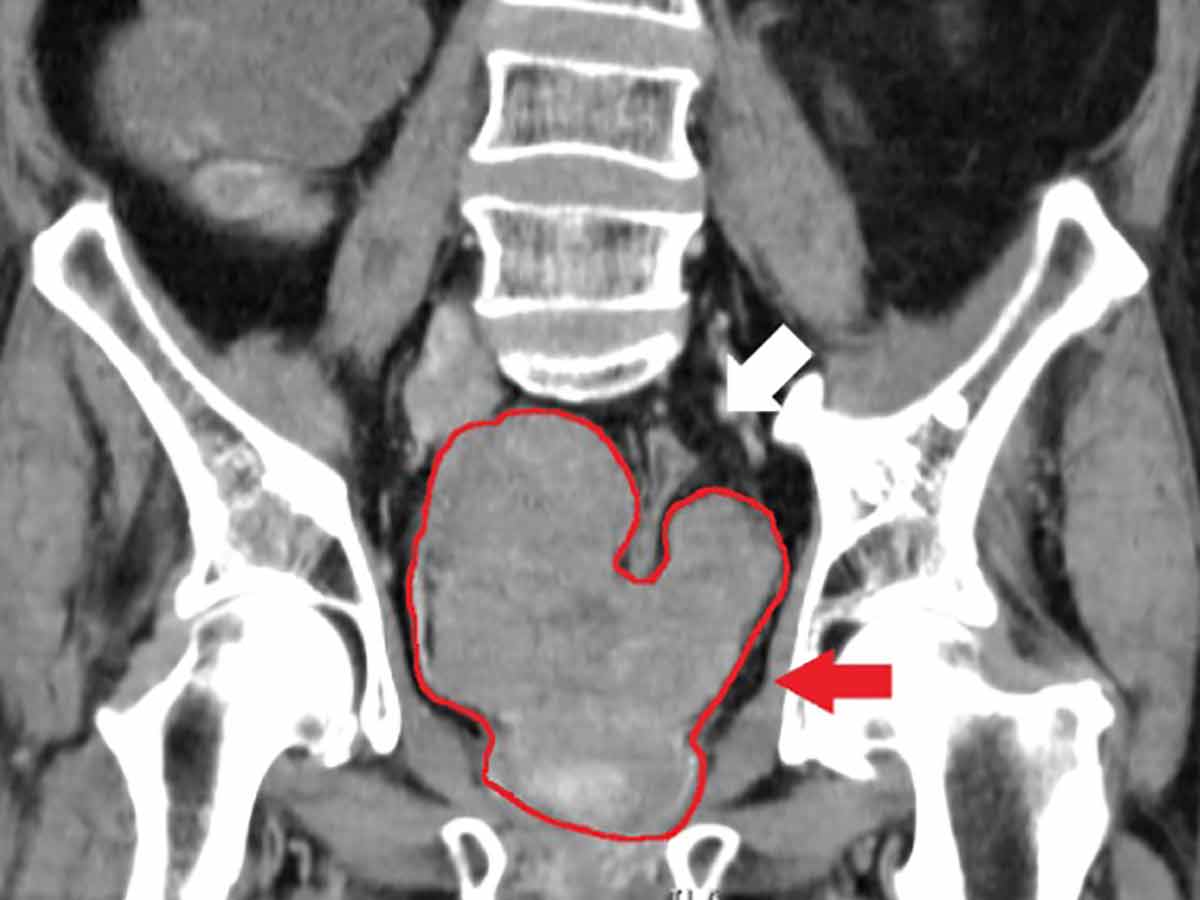
Cancer is scary. It's completely understandable that patients want to take cancer seriously—it can be a devastating and life-ending diagnosis. However, some doctors are starting to argue that it's possible to be too serious and proactive when it comes to detecting and treating some forms of the disease, like prostate cancer.
Prostate cancer, in particular, is often slow-growing and poses no immediate health risks. But that's not to say it should be ignored. Because the risks of prostate removal surgery can include incontinence and sexual problems, many medical professionals support the idea of "watchful waiting" before any drastic measures are taken on a patient.
Hysterectomy

Hysterectomies (the complete removal of the uterus) were once a common treatment option for women experiencing heavy bleeding and severe uterine pain due to fibroids. While effective, no surgery is without risks. Thankfully, we now have much less invasive procedures to help alleviate these problems, such as uterine artery embolization.
While a hysterectomy is not the most high-risk procedure on this list, it's now frequently unnecessary, thanks to newer procedures. So, undergoing one could be a low but pointless risk you don't need to take. That being said, not every woman experiencing these symptoms is a good candidate for these newer procedures, so there may be some instances where a hysterectomy is genuinely necessary.
Hormone Replacement Therapy for Menopause Symptoms
It used to be common practice for women to undergo hormone replacement therapy to help lessen persistent symptoms caused by menopause—like hot flashes, dryness, and trouble sleeping. However, researchers have been uncovering some previously unknown risks associated with this practice which is causing some doctors to rethink prescribing it to menopausal women.
A few studies have now been released that links hormone replacement therapy to things like heart problems and a higher risk of cancer or stroke. For some women with particularly severe symptoms, this may be a risk worth taking, but for others, alternative treatments are worth trying before moving on to HRT.
 Author
Ron Winkler
Last Updated: November 08, 2023
Author
Ron Winkler
Last Updated: November 08, 2023