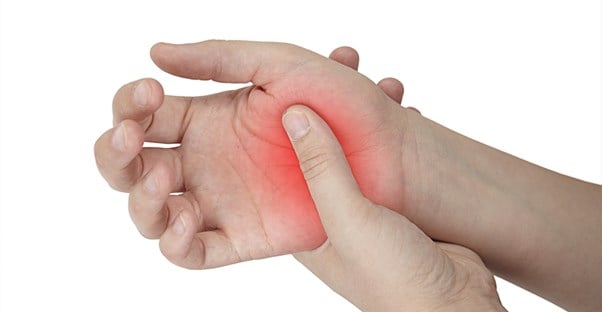
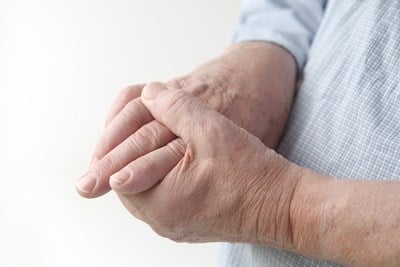
Rheumatoid Arthritis is a chronic disorder resulting from an inflammation of the membranes or tissues that line the joints, typically in the hands and feet, that generally develops in an individual between the ages of forty and sixty.
Over time, rheumatoid arthritis can destroy the cartilage, ligaments, tendons, and bone surrounding the joint. In more severe cases, it may cause damage to organs and other parts of the body, including the skin, eyes, lungs, heart, blood and nerves. Early rheumatoid arthritis symptoms affect the smaller joints in the wrists, hands, and feet, and in most cases the same joints on both sides of the body. This symmetry separates rheumatoid from other types of arthritis and greatly assists in its diagnosis.
The most prominent symptom is joint inflammation, which can cause many uncomfortable conditions including stiffness, swelling, joint pain, tenderness and sensitivity, and swelling and warmth. Clinical diagnosis is based on symptoms, physical exam, x-rays, and labs (blood tests). Typically, a rheumatologist (an expert in autoimmune diseases) performs the diagnosis and long-term management. To manage the complications and reduce risk factors of your rheumatoid arthritis, it's important to recognize problems early and begin appropriate rheumatoid arthritis treatment.
Rheumatoid Arthritis Medical Treatment
Rheumatoid arthritis medical remedies can take on many forms, including medications and surgery intended to relieve symptoms and slow the degenerative process. The type of treatment depends on a person's age, current health, health history, and severity of the arthritis type. Many drugs used to treat rheumatoid arthritis have potentially serious side effects, so doctors tend to prescribe those with the fewest side effects first. As the disease progresses, stronger drugs, and sometimes a combination of drugs, may be necessary.
Common medications include NSAIDs (nonsteroidal anti-inflammatory drugs), corticosteroids (prednisone; methylprednisolone), DMARDs (disease-modifying antirheumatic drugs), immunosuppressants, TNF-alpha inhibitors, and several others that target a variety of inflammatory substances the body produces. Rheumatoid arthritis medical treatment may also come in the form of therapy, which can help one find new and different ways to approach everyday tasks in order to reduce stress off of painful joints. If medications fail to prevent or slow joint damage, one may consider surgery to repair the damaged joints. These surgeries include total joint replacement (arthroplasty), tendon repair, removal of the joint lining (synovectomy), and joint fusion (arthrodesis). Surgery carries a risk of bleeding, infection, and pain, so this rheumatoid arthritis medical treatment should be considered carefully with a rheumatologist.
Rheumatoid Arthritis Lifestyle and Home Remedies
Rheumatoid arthritis lifestyle and home remedies involve steps one can take in order to care for his or her body when living with the disease. These self-care measures, when used side-by-side with medical treatment, can help manage signs and symptoms. Over-the-counter drugs are available, as both pills (aspirin, ibuprofen, naproxen) and topical creams, to help relieve joint pain and reduce swelling and stiffness. Gentle exercise strengthens the surrounding muscles and fights fatigue. One can consult with a physician or seek out classes at public pools or health clubs to find an appropriate exercise program.
Heat can help ease the pain and stiffness associated with rheumatoid arthritis. Taking a hot shower or bath may help. Hot packs and electric heating pads set to low can provide relief to a more concentrated area. Adversely, cold packs and soaking in ice water may dull the pain and have a numbing effect, as well as decrease muscle spasms. One may use both, alternating warm and cold water every few minutes. Finally, one of the best rheumatoid arthritis home remedies is to relax and find ways to cope with pain by reducing life stress. Hypnosis, guided imagery, deep breathing and muscle relaxation are known to control pain.